What to expect
GETTING STARTED WITH A NEW FEEDING TUBE
If you or a loved one are new to tube feeding, we want to help you gain insights on what to expect with useful information for moving through the tube feeding journey.
Understanding the Procedure
VIEW PROCEDURESDischarge from the Hospital
VIEW ARTICLESAt-Home Support
VIEW HELP & RESOURCESManaging Daily Life
VIEW ARTICLESJoin a Support Community
VIEW MIC-KEY CARESTUBE PROCEDURES
Click on the different tube types to understand what to expect with the different procedures.
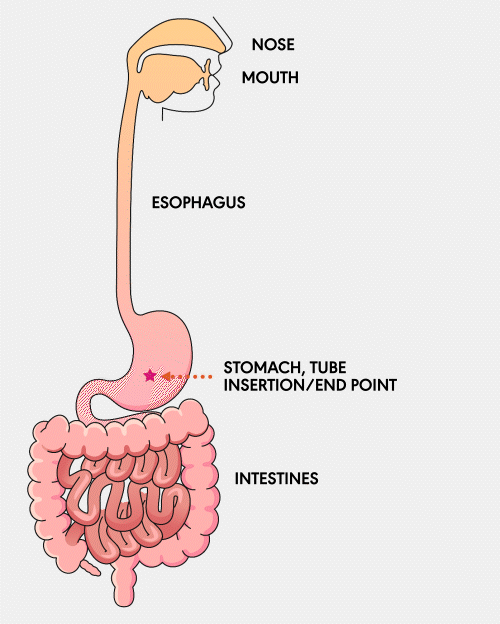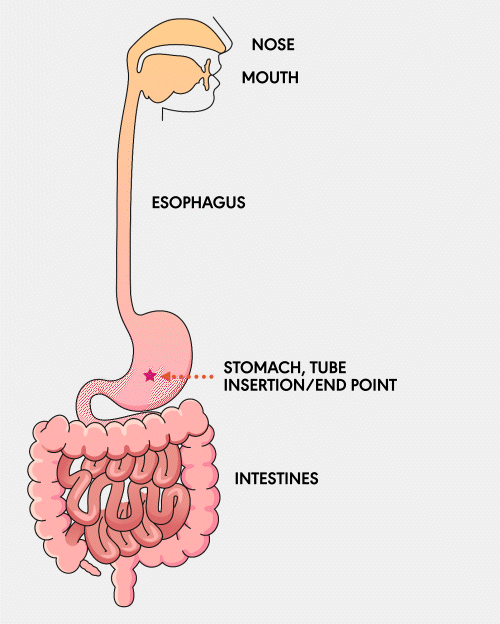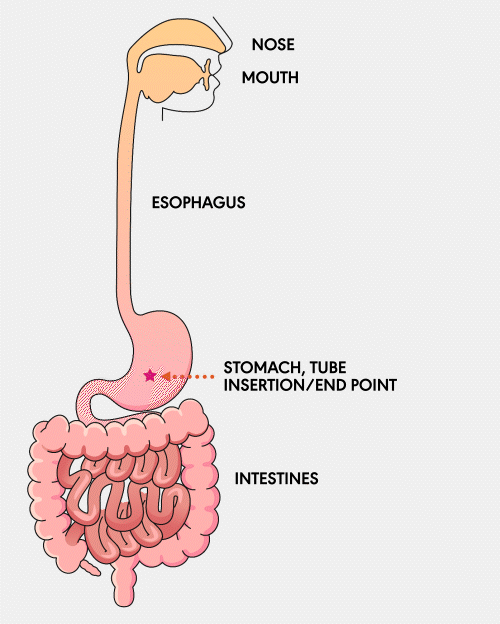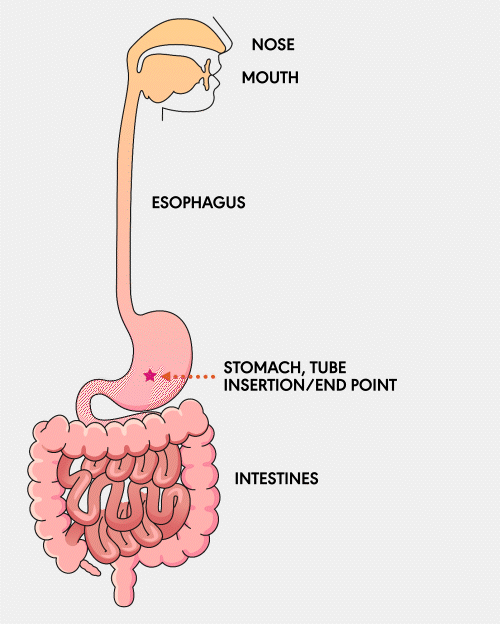
GASTROSTOMY (G) TUBE
A Gastrostomy (G) feeding tube is a tube that is surgically inserted directly into the stomach through the abdominal wall. It is used for individuals who require long-term nutritional support. This tube allows for the direct delivery of nutrients, fluids, and medications into the stomach, ensuring patients receive the necessary sustenance.
Learn More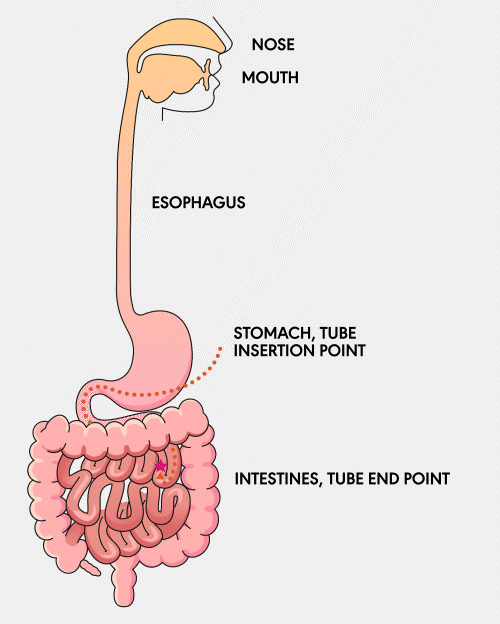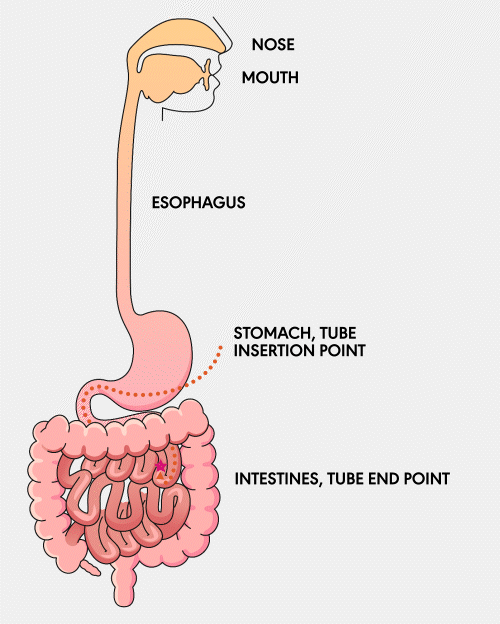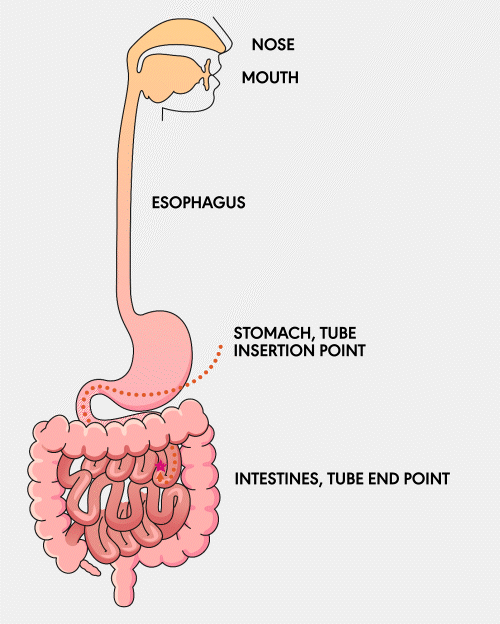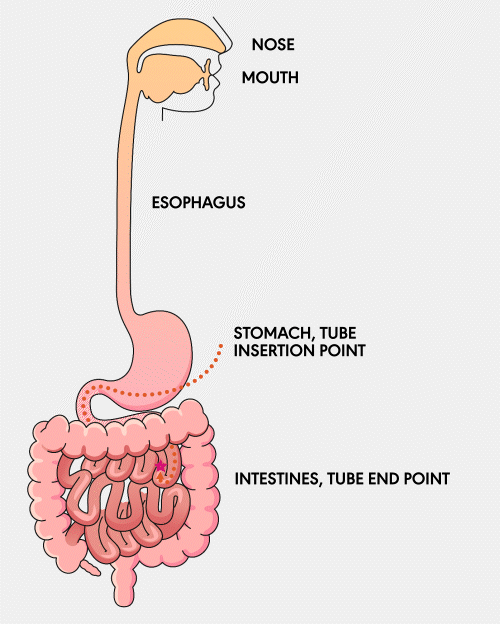
Gastro-Jejunal (GJ) Tube
A Gastro-jejunal (GJ) feeding tube is a tube that is surgically inserted into the stomach and extends into the jejunum, a part of the small intestine. This tube allows for the direct delivery of nutrients, fluids, and medications into the small intestine and access to the stomach for decompression.
Learn More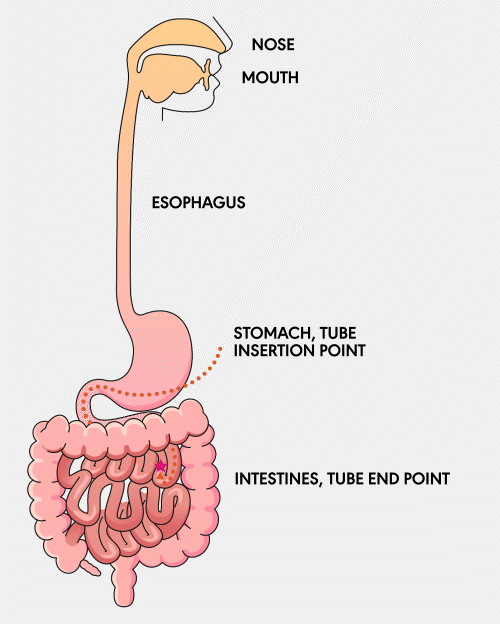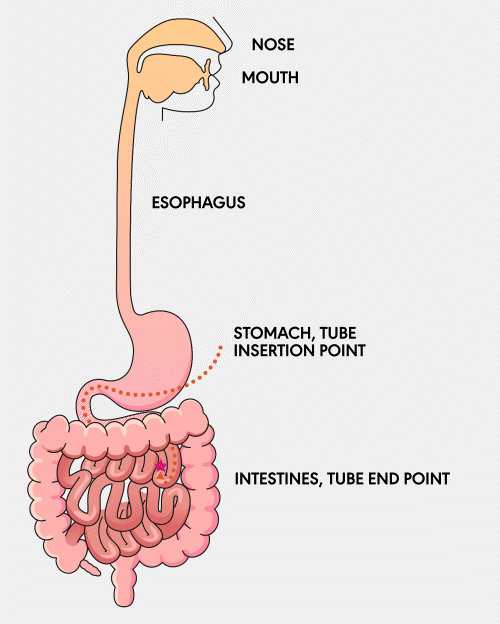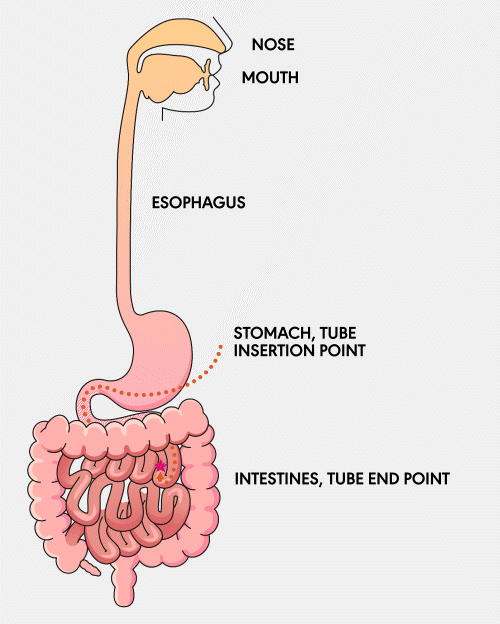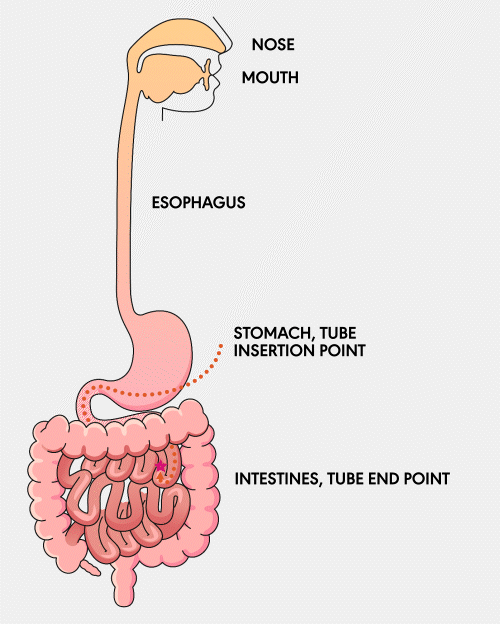
Jejunal (J) Tube
A Jejunal (J) feeding tube is a tube that is surgically inserted into the stomach and extends into the jejunum, a part of the small intestine. It is used with individuals who require long-term nutritional support and cannot tolerate feeding into the stomach.
Learn More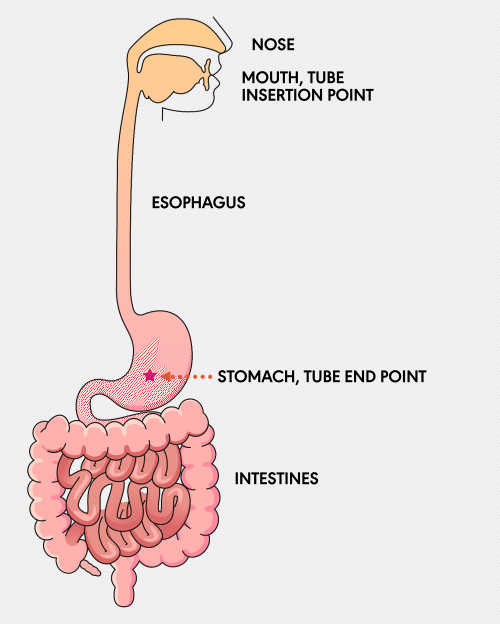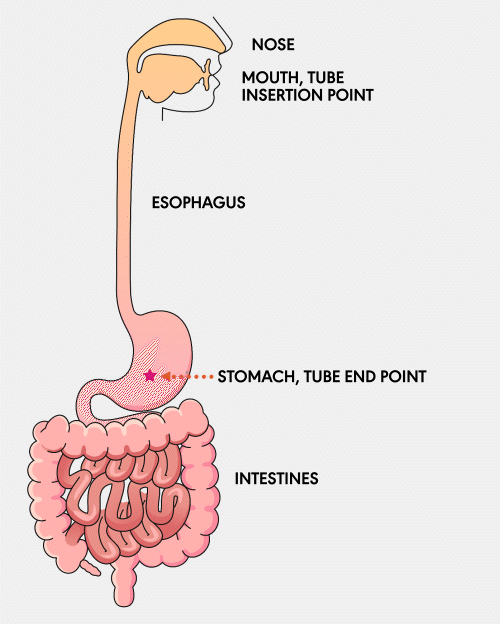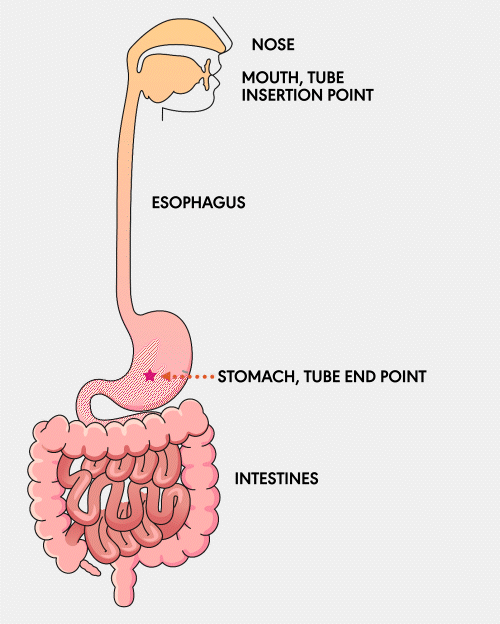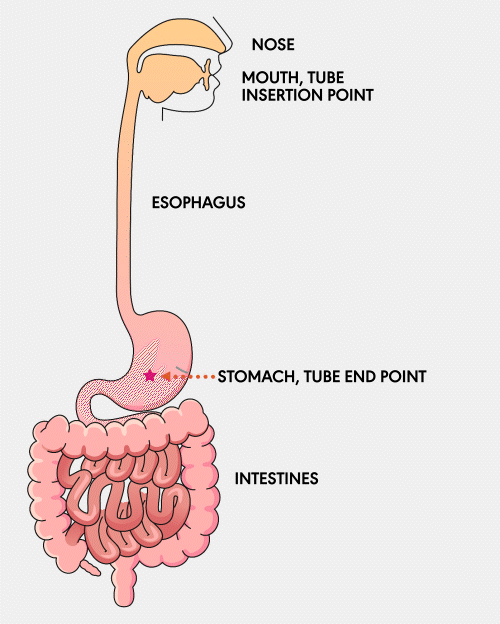
PEG Tube
A Percutaneous Endoscopic Gastrostomy (PEG) feeding tube is inserted into the stomach using an endoscopic procedure. It is used to deliver essential nutrients, fluids, and medication into the stomach.
Learn More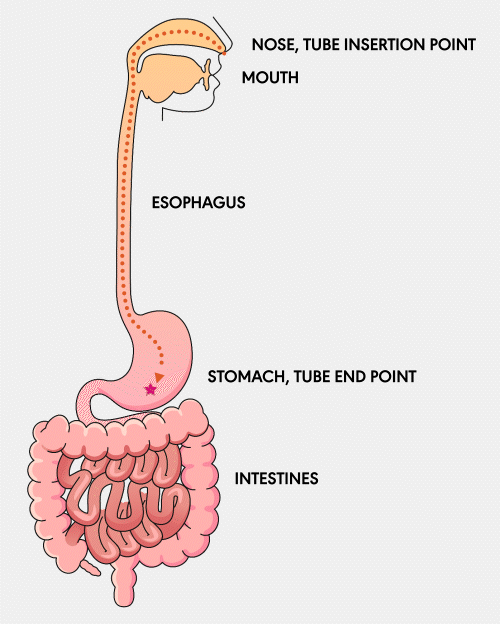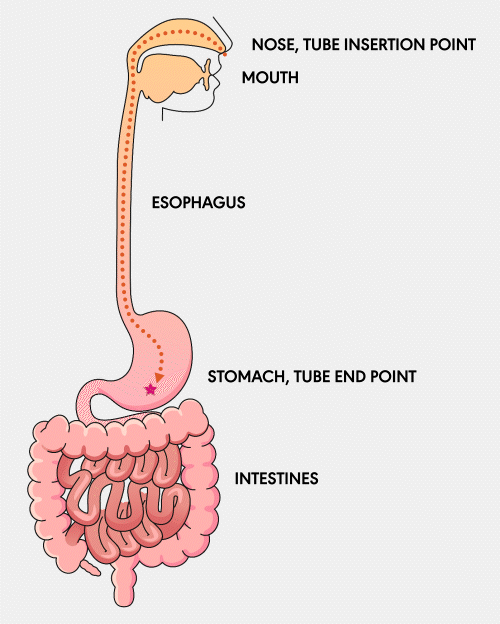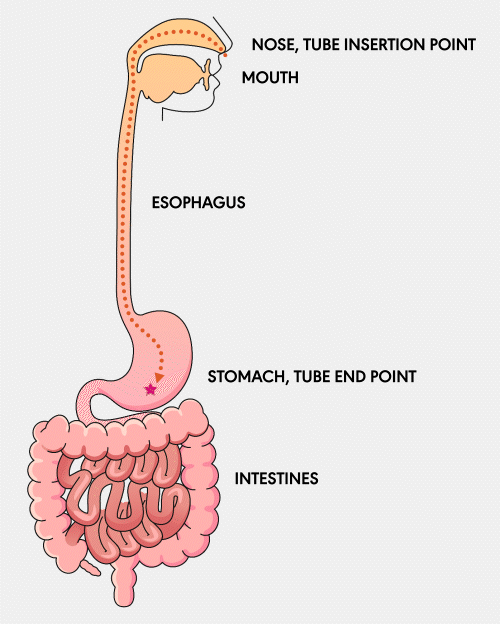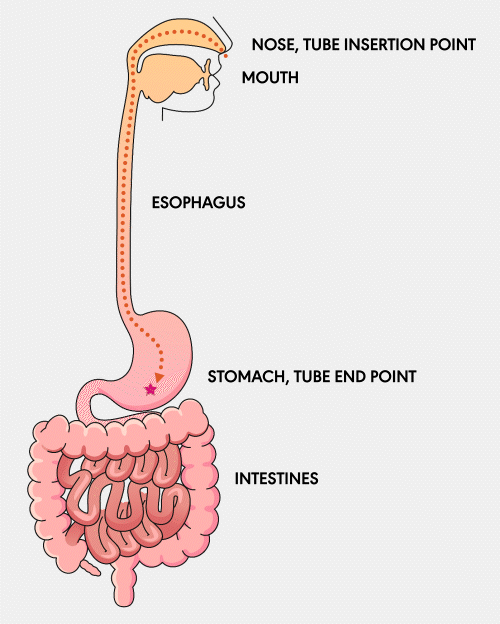
NG Tube
A Nasogastric (NG) feeding tube is a thin, flexible tube inserted through the nose and down into the stomach. This type of tube is typically used for short-term feeding and can be easily inserted and removed by healthcare professionals.
Learn More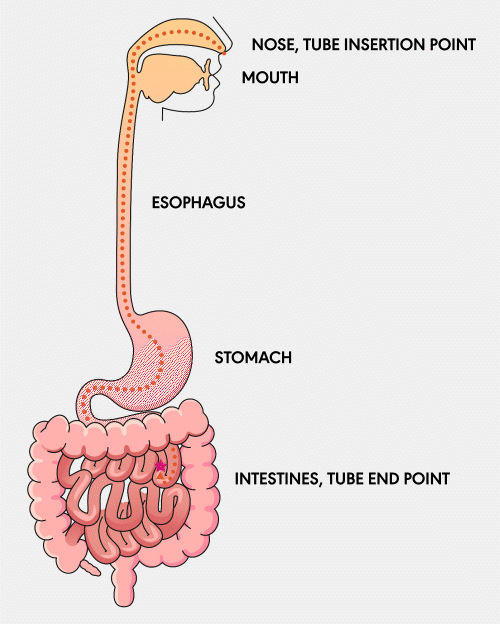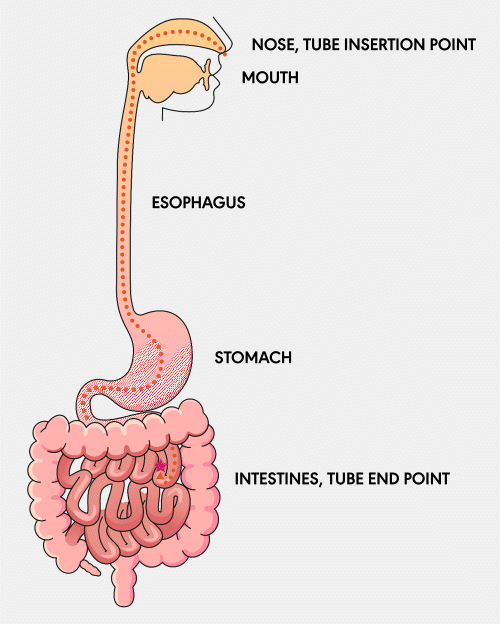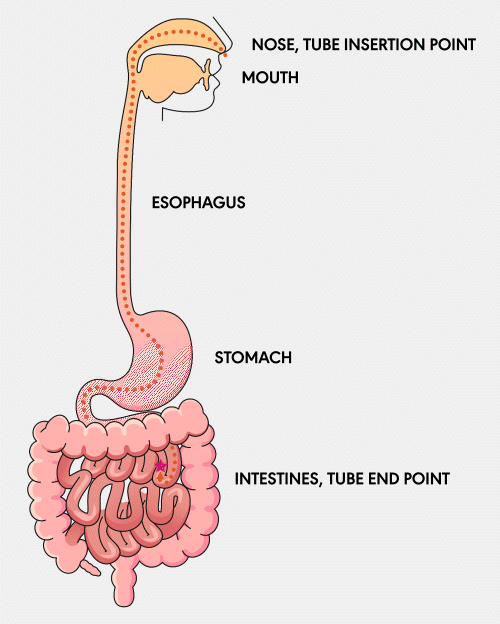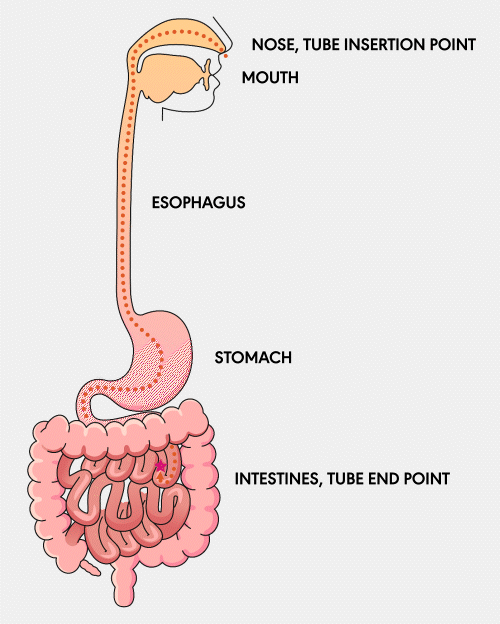
NJ Tube
A Nasojejunal (NJ) feeding tube is a thin tube inserted through the nose, passed through the stomach, and into the jejunum, which is part of the small intestine. This type of tube is often used for feeding patients short-term when the stomach cannot tolerate nutrition.
Learn MoreHelp & Resources

Having a feeding tube can bring about profound changes in one’s life. That’s why we’ve established MIC-KEY* Cares, a complimentary support program and community.
Join MIC-KEY Cares


